Guest Post
Ainsley's Endo Story
by Ainsley Clee-Harris
Ainsley shares her story of heartbreak and hope as she fought to find answers and support for her chronic endometriosis pain and recurrent pregnancy loss.
The battle to be heard and diagnosed
For as long as I can remember I have been in chronic pain. Throughout highschool I missed weeks at a time with excruciating pain, heavy bleeding and migraines.
I was lucky enough to have a very supportive mother. With many women in our family suffering from the same issues as myself, my mother took me seriously – but unfortunately, a lot of doctors did not. My mother and I would go to the GP and she would be told “she is doing this to get out of school”, “there has to be other reasons she is not wanting to leave the house” or “we will put her on the contraceptive pill and that will solve everything”. Luckily for me my mother would not listen and kept fighting and taking me to new doctors to try and get someone to listen.
I suffered from the age of 14 through to 20 trying pills, pain management, the Implanon and even teas and before a new doctor said this was not made up and gave me a referral for a gynaecologist – little did we know it was just going to get more ridiculous.
My first laparoscopy
My first gynaecologist was a middle-aged man who was rude and not very good at listening to his patients. He told me that there is no way I had endometriosis and that I should just go on the pill again. But due to being a migraine sufferer, there were risks associated with being on the contraceptive pills, so he then said I should look into getting a hysterectomy if I didn’t want to be in pain anymore – I was 20 years old!
I went back multiple times, had internal ultrasounds (where he told me he could see nothing to suggest endo) but we eventually got him to agree to put me on the waiting list for surgery.
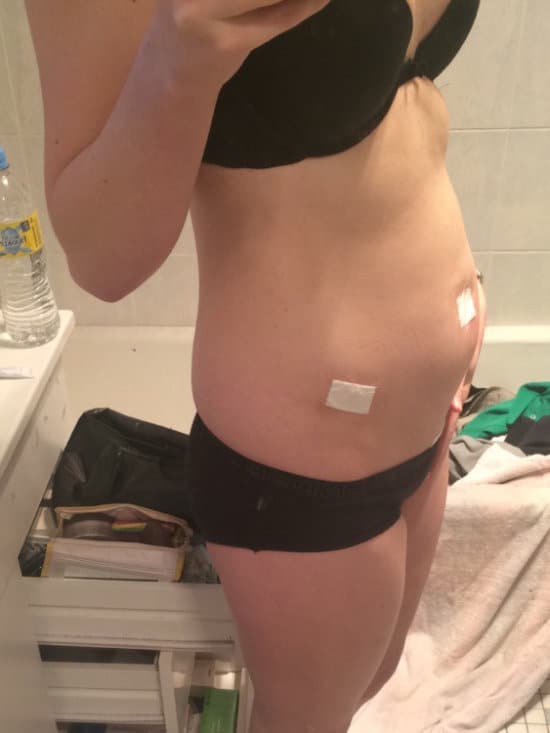
My date finally came up and I had my first laparoscopic surgery – where he found endometriosis and cysts. It was supposed to be a 45-minute scheduled surgery, but I was still in there hours later. It was 6 hours before they came and told my mother what had happened. We never saw that gynaecologist again, didn’t receive any updates or anything after my surgery, and I had a reaction to the anaesthetic, so it was pretty traumatic.
Finally, a diagnosis
I was then told by another doctor at the hospital they found stage 3 endometriosis and removed it from my uterus, fallopian tubes, bowel, bladder and kidneys. At that, I burst into tears because finally there was proof and they had to believe me!
I had a good six months after that. My migraines had settled and period pain was manageable, but then it all went south in my private life. I had a bad boyfriend and was physically and mentally abused, but I somehow got a miracle through all the bad and fell pregnant. I decided to leave my abuser and I ended up losing my baby.
My second laparoscopy
My pain started to get worse three months after my first “normal” cycle. (Normal isn’t a word I like to use because for me I never had one that anyone would deem normal). I had somehow managed to meet the love of my life and he encouraged me to continue to get help for my pain. In the next twelve months, my mother and partner were questioned at the local hospital about whether I was addicted to drugs, crying for attention, lonely, or trying to end my life. It wasn’t until one doctor turned around and told my mother “you should have raised her better” that a fire started back up inside of me.
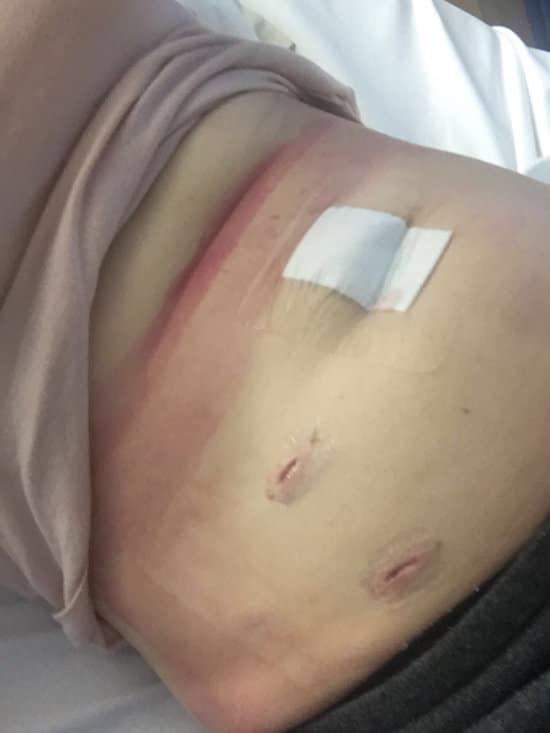
I sought out another gynaecologist, This one was two hours away and highly recommended, but being a private practice it was quite expensive. She was lovely and so incredible, she was aware I wanted children so put me on the waiting list for another surgery, and I got in with a cancellation. She found stage 2 endometriosis stage and cysts on my ovaries.
Starting fertility treatment
I then began fertility treatment, and sadly we were not successful. We tried to just live life and work, and decided if it was meant to be then hopefully it would happen. I ended up surprisingly falling pregnant but unfortunately ended with another loss.
I was taken to a hospital an hour away for scans and was bawling on the phone to my father, as I was put into a maternity ward and I could hear babies crying and mothers settling their little ones. I was saying “I can’t be here, I can’t! It’s not fair”, when a nurse walked in and told me I shouldn’t be so ungrateful as I was getting health care when others weren’t so lucky. I left the hospital a different person, and I was going to be stronger.
I went off all pain medication and tried natural methods, as well as started a healthier lifestyle. It was so hard.
Third time lucky
I sought out another gynaecologist that I was told about and he really changed my life! I walked into my first consultation and said: “Don’t beat around the bush, tell me straight because I know I have endo and I want a family and I need your help”. He did an internal ultrasound and saw that I was pregnant, but due to my likelihood of an unsuccessful pregnancy told me to not get my hopes up. I unfortunately miscarried a week later. We did blood tests and I was put on a waiting list – and then Covid hit!
He was such an incredible man that he did all his public surgeries pro-bono at a private day surgery unit, as all reproductive treatments had been deemed “elective surgeries”. I had lost my job due to Covid, so we went to my parents and they helped with getting money organised to pay for the day surgery stay and anaesthetist.
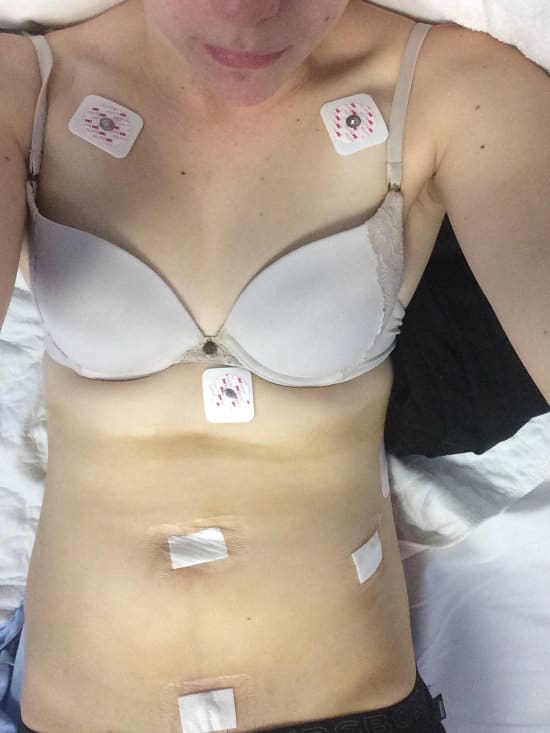
Afterwards, at my check-up, he told me he found stage 3 endometriosis, adenomyosis and fibroid tumours. He said to do everything he told me and he would get me pregnant in three months. I was sceptical.
Month after month passed and we were heartbroken. But on my third round of fertility treatment, I fell pregnant and we got our rainbow!
I’m now 28 and we are about to start the process again to try and have a second child.



Unfortunately, stories like Ainsley’s are all too familiar. That’s why we’re fighting so hard to improve endometriosis care for everybody. No one should ever be made to feel crazy or have to wait YEARS just to get a diagnosis and treatment, especially when endo is so common that it affects 1 in 9 women and people with a uterus. Our annual Walk4Endo fundraising event aims to raise money and awareness for endo research, and we’re constantly looking at new ways to improve things for all the endo warriors of today and generations to come.

Guest Post: Ainsley’s Endo Story
Ainsley shares her story of heartbreak and hope as she fought to find answers and support for her chronic endometriosis pain and recurrent pregnancy loss.

Guest Post: Menopause Reflections – by Jadie Hunter
Finally, menopause is out there on social media, and it is no longer a taboo subject – remember, it impacts half the population. Here’s Jadie’s story of medically-induced menopause.

Walk the World 4 Endo Projects
Our first Walk The World 4 Endo was a great success. We had hundreds of walkers take part. As a collective, we walked 13, 588km